-
Fil d’actualités
- EXPLORER
-
Pages
-
Groupes
-
Evènements
-
Blogs
-
Offres
-
Emplois
-
Cours
Billing Services for Mental Health Clinics in USA: Complete Guide to Compliance and Revenue Growth
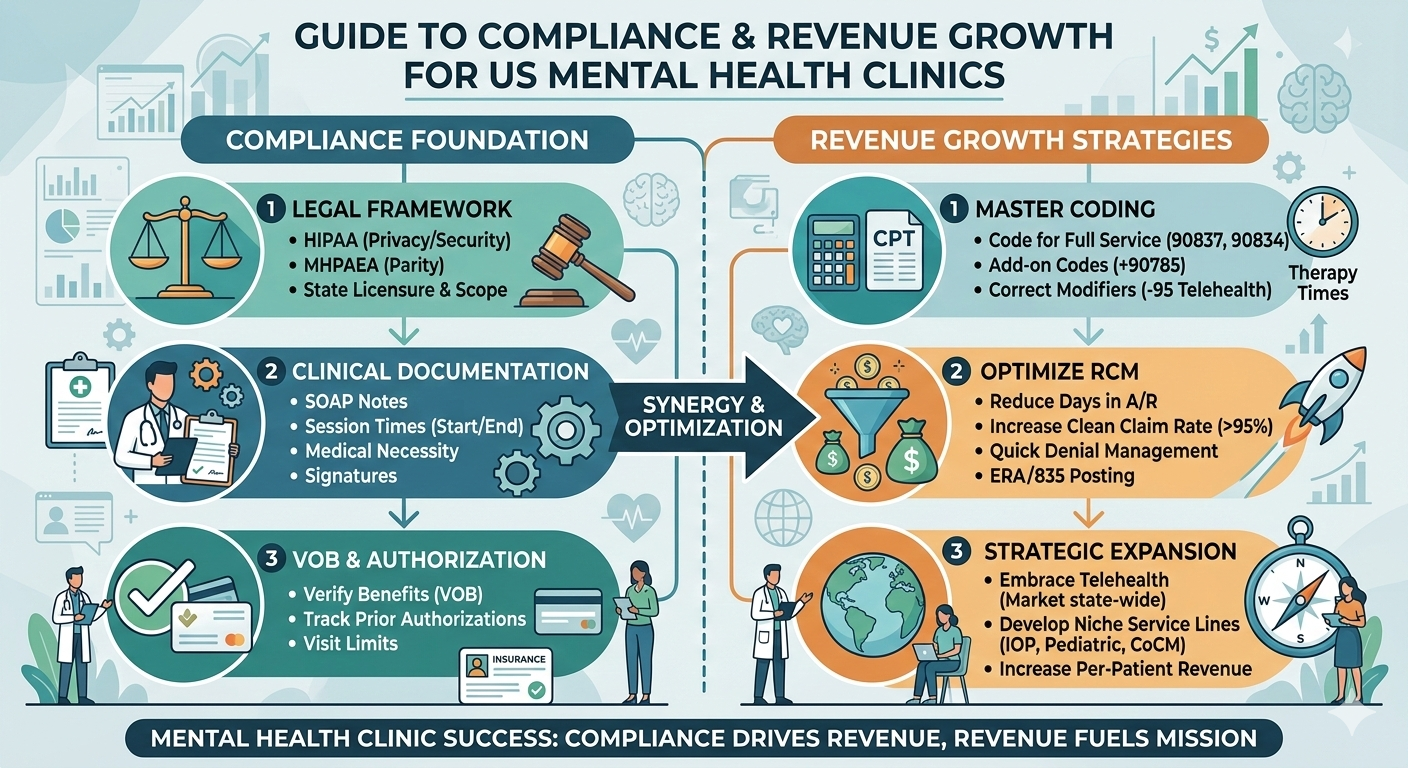
Mental health practices across the United States are facing increasing administrative pressure. Reimbursement rules change frequently, payer policies vary by state, and documentation standards are more detailed than ever. For many clinic owners, managing claims has become as challenging as delivering quality care.
That is why billing services for mental health clinics are no longer considered optional support. They are a strategic tool for financial stability and compliance.
Before exploring how professional support can help, here is what mental health clinics in the USA are currently dealing with:
-
Increasing claim denials from commercial and government payers
-
Strict documentation requirements for therapy and psychiatry services
-
Complex coding updates and modifiers
-
Growing demand for telehealth billing accuracy
-
Delays in credentialing and payer enrollment
-
Medicare and Medicaid compliance risks
This guide explains how mental health billing services work, what to look for in a partner, and how clinics can protect revenue while focusing on patient care.
Why Billing for Mental Health Clinics Is More Complex Than Other Specialties
Mental health billing involves far more than submitting CPT codes. Clinics must understand psychotherapy time-based coding, medication management billing, evaluation and management documentation, and payer-specific requirements.
Billing for mental health services also requires familiarity with:
-
Telepsychiatry reimbursement policies
-
Authorization requirements
-
Incident-to billing rules
-
State parity laws
-
Coordination with Medicaid managed care plans
Unlike many procedural specialties, mental health claims are highly documentation-driven. Even minor inconsistencies between session time and notes can trigger denials.
Because of this complexity, many providers are turning to mental health billing specialist companies that focus exclusively on behavioral healthcare reimbursement.
What Are Billing Services for Mental Health Clinics?
Billing services for mental health clinics refer to outsourced or managed revenue cycle support tailored specifically to therapists, psychologists, psychiatrists, and behavioral health facilities.
These services typically include:
-
Insurance verification and benefits checks
-
Authorization management
-
Coding and billing for mental health services
-
Claim submission and follow-up
-
Denial management and appeals
-
Payment posting and reconciliation
-
Reporting and analytics
A mental health billing company understands the nuances of therapy session documentation, crisis intervention billing, and billing Medicare for mental health services, which often differs from commercial payer policies.
In-House vs Outsourcing Mental Health Billing
Many clinic owners initially attempt in-house billing. While this may work for small practices, growth often exposes operational weaknesses.
In-house challenges include:
-
Staffing shortages
-
Limited payer knowledge
-
Lack of denial tracking systems
-
Compliance risks
-
Training costs
Outsourcing mental health billing allows clinics to transfer these operational burdens to experts. With outsourced billing for mental health, providers gain access to experienced coders, billing specialists, and denial analysts without the overhead of full-time employees.
Outsourcing mental health billing and coding can also improve turnaround time and reduce accounts receivable days when managed correctly.
How a Mental Health Billing Services Company Improves Revenue
A professional mental health billing services company focuses on maximizing clean claim rates and accelerating reimbursements. Their approach typically includes:
Accurate coding
Proper coding ensures correct use of psychotherapy add-on codes, crisis codes, and evaluation and management services.
Documentation audits
Regular audits reduce compliance risks and prevent payer recoupments.
Proactive denial management
Instead of reacting to rejections, strong billing companies for mental health analyze denial trends and correct root causes.
Medicare and Medicaid expertise
Billing Medicare for mental health services requires strict adherence to documentation rules and coverage limitations. Experienced teams prevent costly errors.
Performance tracking
Advanced reporting systems track claim acceptance rates, aging reports, and reimbursement trends.
When executed properly, medical billing for mental health becomes a structured revenue engine rather than a daily struggle.
What to Look for in the Best Mental Health Billing Company
Not all vendors specialize in behavioral healthcare. Choosing the best mental health billing services company requires careful evaluation.
Look for:
Experience in behavioral and mental health billing services
The team should understand psychotherapy codes, psychiatric evaluations, and group therapy billing.
Dedicated account management
A single point of contact improves communication and accountability.
Transparent pricing
Avoid unclear fee structures that increase costs over time.
Credentialing support
Mental health billing and credentialing services help providers enroll with payers and maintain active contracts.
Compliance knowledge
HIPAA compliance and payer regulation awareness are essential.
A top mental health billing company will provide performance reports, denial analytics, and compliance monitoring rather than simply submitting claims.
The Role of Coding in Mental Health Medical Billing
Coding accuracy directly affects revenue. Coding and billing for mental health services must reflect session duration, treatment complexity, and medical necessity.
Common services include:
-
Individual psychotherapy
-
Family therapy
-
Group therapy
-
Psychiatric evaluations
-
Medication management
Billing for mental health therapists often depends on precise time tracking. Undercoding leads to lost revenue, while overcoding increases audit risk.
Mental health billing solutions typically include certified coders who stay updated on CPT and ICD-10 changes.
Credentialing and Its Impact on Reimbursement
Without proper credentialing, even correctly submitted claims will not be paid. Many clinics underestimate how critical enrollment and contract management are.
Mental health billing and credentialing services handle:
-
Initial payer enrollment
-
Revalidation
-
CAQH updates
-
Contract negotiation support
Delays in credentialing can cost clinics months of lost revenue. Partnering with a reliable mental health billing company ensures providers are approved before seeing patients under new insurance plans.
Common Challenges in Billing for Mental Health Providers
Behavioral health clinics frequently encounter:
High denial rates
Mental health claims are often denied for missing documentation or incorrect modifiers.
Telehealth billing confusion
Policies change frequently, especially regarding place of service codes.
Coordination of benefits issues
Many patients have multiple insurance plans.
Medicare compliance risks
Billing Medicare for mental health services requires strict adherence to coverage criteria.
Administrative overload
Small clinics struggle with billing mental health services while maintaining patient care standards.
Working with mental health billing specialist companies reduces these operational risks.
Is There a Cheap Outsource Mental Health Billing Company That Delivers Quality?
Cost is an important factor for small practices. While many search for a cheap outsource mental health billing company, price should never be the only decision driver.
Low-cost vendors may:
-
Use inexperienced staff
-
Offer limited denial follow-up
-
Provide minimal reporting
-
Lack compliance monitoring
The best outsource mental health billing and coding services balance affordability with expertise, transparency, and measurable performance improvement.
Instead of focusing only on cost percentage, clinics should evaluate net collection rate, claim acceptance rate, and average reimbursement time.
How Outsourced Billing for Mental Health Supports Growth
As clinics expand into multiple providers or locations, billing becomes more complex.
Outsourced billing for mental health supports scalability by:
-
Standardizing workflows
-
Reducing claim errors
-
Managing payer contracts
-
Providing revenue forecasting
-
Improving patient billing transparency
Professional billing services for mental health create predictable cash flow, allowing clinic owners to invest in staff, marketing, and patient care.
Technology and Reporting in Modern Mental Health Billing
Advanced mental health billing solutions integrate with electronic health record systems to reduce errors.
Key features include:
-
Automated eligibility checks
-
Real-time claim status tracking
-
Electronic remittance posting
-
Custom financial dashboards
Billing for mental health becomes more efficient when supported by analytics that highlight denial trends and payer performance.
Choosing the Right Mental Health Billing Partner in the USA
When evaluating a mental health billing services company, consider:
-
Years of experience in mental health medical billing
-
Knowledge of state-specific Medicaid policies
-
Medicare expertise
-
References from behavioral health clients
-
Reporting transparency
-
HIPAA compliance practices
The best mental health billing company will act as a long-term revenue partner rather than a transactional vendor.
How 247 Medical Billing Services Supports Mental Health Clinics
For clinics seeking comprehensive support, 247 Medical Billing Services provides integrated solutions tailored to behavioral healthcare providers across the USA.
Their offerings include medical billing services, medical coding services, and complete medical billing and coding services designed specifically for mental health practices. They also provide revenue cycle management to improve cash flow and reduce denials, along with credentialing services to ensure providers are properly enrolled with commercial and government payers.
By combining billing for mental health clinics with compliance oversight and performance tracking, clinics gain a structured approach to revenue growth.
Conclusion
Billing services for mental health clinics play a vital role in protecting revenue, ensuring compliance, and reducing administrative stress. As reimbursement rules grow more complex, relying on experienced mental health billing specialist companies becomes a strategic advantage rather than an expense.
Whether through outsourcing mental health billing or partnering with a full-service mental health billing company, clinics that invest in expert support position themselves for sustainable financial growth while focusing on patient care.
Frequently Asked Questions
What are billing services for mental health clinics?
Billing services for mental health clinics manage insurance verification, coding, claim submission, denial follow-up, and payment posting specifically for behavioral healthcare providers.
Why should clinics consider outsourcing mental health billing?
Outsourcing mental health billing reduces administrative burden, improves claim accuracy, lowers denial rates, and ensures compliance with Medicare and commercial payer requirements.
How is billing for mental health services different from other specialties?
Billing for mental health services is highly documentation-driven, often time-based, and subject to strict medical necessity guidelines, particularly when billing Medicare for mental health services.
Do mental health billing companies handle credentialing?
Many mental health billing and credentialing services include payer enrollment, CAQH management, and contract maintenance to ensure providers can receive reimbursements.
How do I choose the best mental health billing services company?
Look for experience in behavioral and mental health billing services, transparent pricing, strong reporting systems, compliance knowledge, and proven success with mental health providers in the USA.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jeux
- Gardening
- Health
- Domicile
- Literature
- Musique
- Networking
- Autre
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


